 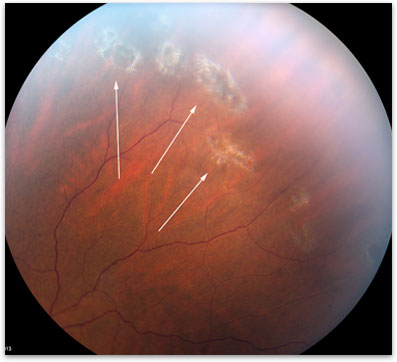
Often the thinning becomes so profound that a full-thickness hole atrophies through the retina at the lattice lesion. The retinal thinning has several effects: (1) the overlying vitreous will be disturbed, resulting in a pocket of liquefaction overlying the lattice lesion known as a lacuna (2) the vitreous along the edges of the lattice lesion will undergo strong adhesion to the retina and (3) the ischemia and retinal thinning will disturb the retinal pigment epithelium, resulting in RPE hyperplasia and a pigmented appearance. There is sclerosis of the larger vessels, with their lumen being filled with extracellular glial tissue, giving lattice degeneration its characteristic fibrotic appearance. It appears to be due to dropout of peripheral retinal capillaries with resulting ischemia, which induces thinning of all retinal layers. Lattice degeneration is typically bilateral. A tractional linear tear will occur on the posterior edge of lattice lesions in 1.9 percent of lesions. The incidence of atrophic holes in lattice degeneration ranges from 18 to 42 percent. Atrophic holes are often present in the lesion, occasionally large enough to encompass the entire lattice lesion. There may be associated RPE hyperplasia, giving the lesion a pigmented appearance. The individual lesions are usually from one-half to six disc diameters and may run 360 degrees around the eye in a discontinuous pattern. It nearly always runs circumferentially between the equator and the ora serrata. It presents as a linear trail of fibrosed vessels within atrophied retina in a "lattice" pattern. Lattice degeneration occurs in eight to 11 percent of the general population. There is no racial or sexual predilection. There appears to be a higher incidence of myopia in patients with lattice degeneration. Mutations in COL111A2 can give rise to a syndrome with the systemic features of Stickler syndrome but no ophthalmological abnormality.The patient is usually over age 20 and is nearly always asymptomatic, except for possible complaints of flashing lights (photopsia). The remainder with the type 2 vitreous phenotype have mutations in COL11A1 or other loci yet to be identified. The majority of families with Stickler syndrome have mutations in the COL2A1 gene and show the characteristic type 1 vitreous phenotype. Mitral valve prolapse was reported to be a common finding in one series but not in our experience. Stature and intellect are usually normal. Occasional findings include slender extremities and long fingers. Sensorineural deafness with high tone loss may be asymptomatic or mild. Mild spondyloepiphyseal dysplasia is often apparent radiologically. Osteoarthritis develops typically in the third or fourth decade. There is joint hypermobility which declines with age. Midline clefting, if present, ranges in severity from a cleft of the soft palate to Pierre-Robin sequence. These features can become less pronounced with age. Children with Stickler syndrome typically have a flat midface with depressed nasal bridge, short nose, anteverted nares, and micrognathia. Non-ocular features show great variation in expression. Less common ophthalmological features include paravascular pigmented lattice degeneration and cataracts. There is a substantial risk of retinal detachment. Abnormalities of vitreous gel architecture are a pathognomonic feature, usually associated with high myopia which is congenital and non-progressive. Stickler syndrome is an autosomal dominant disorder with characteristic ophthalmological and orofacial features, deafness, and arthritis. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
